NB hiPSC lung models; Valuable tools in understanding health impacts of air pollution
Lung cancer is one of the most common cancers in urban populations.6 Diesel engine exhaust, outdoor air pollution and particulate matter have all been classified by the WHO as carcinogenic to humans.10
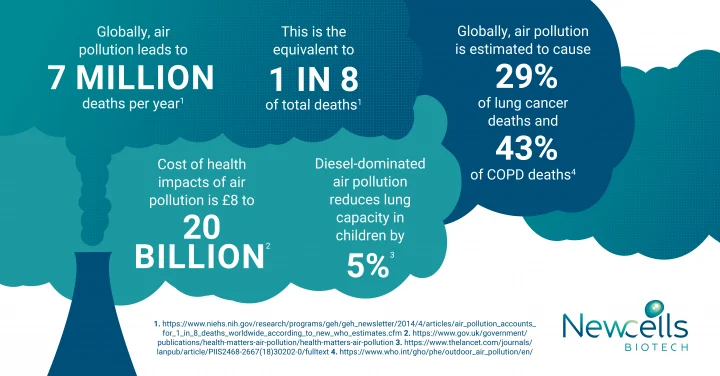
Data from the Global Burden of Disease Project indicated that in 2010, there were 223,000 lung cancer deaths resulting from air pollution. Data from 2016 showed that worldwide, ambient air pollution is estimated to cause about 16% of lung cancer deaths.5
In response to these risks, in 2016, the UK government called for Clean Air Zones (CAZ) in city centres in an attempt to “improve the urban environment to support public health and the local economy, making cities more attractive places to live, work, do business and spend leisure time”.11 Under the plans, CAZ will be introduced in Birmingham, Leeds, Nottingham, Derby and Southampton by 2020. Similar strategies have since been proposed in other city centres, including Newcells Biotechs’ hometown Newcastle-upon-Tyne. CAZ will see the most polluting vehicles, such as old buses, taxis, coaches and lorries, discouraged from entering the zone through charges.
Despite this, Asthma UK suggest that as the plans don’t include cars, it is highly unlikely that they will significantly improve air quality and health.12 In addition, Low Emission Zones implemented in London have improved air quality, but there is no evidence that they have helped improve children’s respiratory health. 7
It is therefore essential that we continue to increase our understanding of how air pollution affects the human body and in particular the lungs. Newcells’ lung organoids have the potential to be valuable to tool to researchers in this field.
References
- World Health Organisation. 7 million premature deaths annually linked to air pollution. Available from: https://www.who.int/mediacentre/news/releases/2014/air-pollution/en/ [Accessed 25 Jul 2019]
- GOV.UK. Health matters: air pollution. Available from: https://www.gov.uk/government/publications/health-matters-air-pollution/health-matters-air-pollution [Accessed 25 Jul 2019]
- Abbey, D. E. Burchette, R. J. Knutsen, S. F. McDonnel, W. F. Lebowitz, M. D. Enright, P. L. Long-term Particulate and Other Air Pollutants and Lung Function in Nonsmokers. American Journal of Respiratory and Critical Care Medicine. 1998. 158(1): 289-98. Available from: https://www.atsjournals.org/doi/10.1164/ajrccm.158.1.9710101
- U.S. Environmental Protection Agency. Air quality index. Research Triangle Park. NC: 2009. Available from: https://www.airnow.gov [Accessed 26 Jul 2019]
- World Health Organisation. Mortality and burden of disease from ambient air pollution. Available from: https://www.who.int/gho/phe/outdoor_air_pollution/burden_text/en/ [Accessed 29 ul 2019]
- Jiang, X-Q. Mei, X-D. Feng, D. Air pollution and chronic airway diseases: what should people know and do? Journal of Thoracic Disease. 2016. 8(1): E31–E40. Available from: https://jtd.amegroups.org/article/view/5951/6192 [Accessed 26 Jul 2019]
- Mudway, I.S. Dundas, I. Wood, H.E. Marlin, N. Jamaludin, J.B. Bremner, S.A. Cross, L. Grieve, A. Nanzer, A. Barratt, B.M. Beevers, S. Dajnak, D. Fuller, G.W. Font, A. Colligan, G. Sheikh, A. Walton, R. Grigg, J. Kelly, F.J. Lee, T.H. Griffiths, C.J. Impact of London’s low emission zone on air quality and children’s respiratory health: a sequential annual cross-sectional study. Lancet Public Health. 2019. 4(1):e28-e40. Available from: https://doi.org/10.1016/S2468-2667(18)30202-0
- Liu, Y. Xu, J. Chen, D. Sun, P. Ma, X. The association between air pollution and preterm birth and low birth weight in Guangdong, China. BMC Public Health. 2019. 19: 3. Available from: https://doi.org/10.1186/s12889-018-6307-7
- Oudin, A. Bråbäck, L. Oudin Åström, D. Strömgren, M. Forsberg, B. Association between neighbourhood air pollution concentrations and dispensed medication for psychiatric disorders in a large longitudinal cohort of Swedish children and adolescents. BMJ Open. 2016. 6: e010004. Available from: http://dx.doi.org/10.1136/bmjopen-2015-010004
- GOV.UK. Understanding the impact of particulate air pollution. Available from: https://ukhsa.blog.gov.uk/2015/11/03/understanding-the-impact-of-particulate-air-pollution/ [Accessed 29 Jul 2019]
- GOV.UK. Air quality: clean air zone framework for England. Available from: https://www.gov.uk/government/publications/air-quality-clean-air-zone-framework-for-england [Accessed 29 Jul 2019]
- Asthma UK. Implementation of Clean Air Zones in England.
Share on social media:
Don't miss out on our latest innovations: follow us on Linkedin



