Why is an in vitro model of the glomerulus desperately needed?
Kidney failure is a leading cause of death, causing more death than breast or prostate cancer. The main causes of kidney failure are diabetes, high blood pressure, inherited diseases such as polycystic kidney disease and glomerulonephritis, diseases that damage the kidney’s filtering units or glomerulus.
In most cases, once the kidney’s function is limited, the only treatment options are dialysis and kidney transplant. The absence of effective drugs to treat kidney disease is partly due to the lack of physiologically relevant models of the glomerulus.
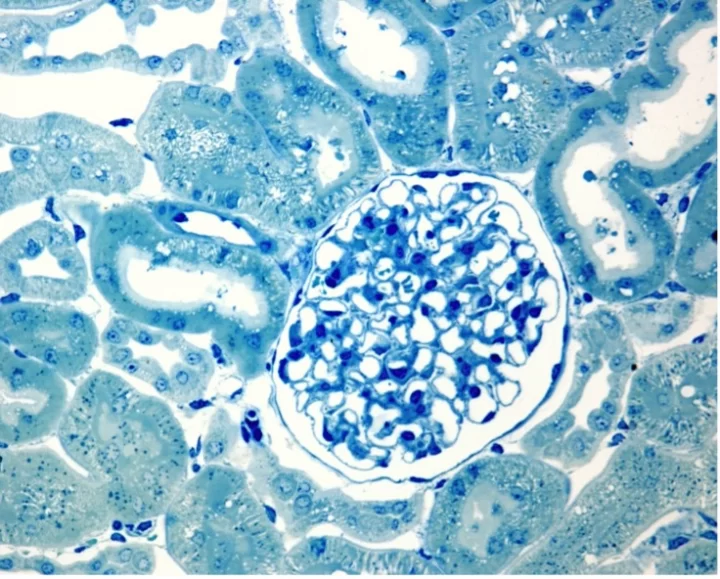
While a suitable in vitro model of the glomerulus is desperately needed, it is a challenge to recapitulate the complex glomerular structures. The glomerulus is a network of capillaries located within the nephron that filtrates small solutes out of the blood by pressure. These capillaries are lined by endothelial cells with gaps between them (so-called fenestrae) to allow water and solutes to exit the vascular system and pass through the glomerular basement membrane, epithelial cells, or podocytes.
Blood runs into the capillaries from the afferent arterioles and, unlike most capillary structures, the glomerular capillaries exit into efferent arterioles. This provides a tighter control over the blood flow, allowing the glomerulus blood pressure to remain high independently of other factors affecting systemic blood pressure. The higher glomerular blood pressure and specialized membranes in the afferent arteriole allow the extraction of most solutes from the blood in the process known as glomerular filtration. The endothelial cells, the glomerular basement membrane and the podocytes constitute the glomerular filtration barrier (GFB). All solutes in the glomerular capillaries, except for macromolecules like proteins, get filtrated by passive diffusion.
The glomerular filtration rate (GFR) is the volume of glomerular filtrate formed per minute by the kidneys. The GFR is regulated by multiple mechanisms, and it usually reduced in kidney disease. Within the glomerular filtration barrier, specialised epithelial cells called podocytes, which are composed of composed of large cell body and major extending processes. Those form the size selective sieve, with their long finger-like projections wrapping around the blood vessels. Specific genes, such as nephrin, podocin, synaptopodin, Wilms tumour protein (WT1) and podocalyxin are specific to podocytes and are crucial for the maintenance of the glomerular filtration barrier (GFB). Damage to podocytes is equivalent to holes in the sieve resulting in larger and essential compounds such as proteins being lost from the blood into urine (proteinuria) instead of being retained.
The scientific community has been longing for a reliable podocyte model. Newcells has been working hard to develop a new robust in vitro model of the glomerulus that contains a pure population of primary human podocytes, which are isolated from fresh healthy human kidneys and express all the key marker proteins. As a result, this new model is functional and physiologically relevant. Newcells in vitro glomerulus model will soon be available in 96-well plates and exhibits filtration size selectivity comparable to that observed in vivo, indicating its suitability for drug screening, assessment of drug safety and efficacy and glomerular disease modelling.
Newcells offers a high quality and reliable service for the evaluation of customer compounds carried out by our experienced scientists. We develop and complete study protocols in our laboratories in the UK, working closely with our customers to define a tailored study design that best delivers the required data outputs.
For details on the type of assays we are developing for the glomerular model, watch our webinar on Developing High Content Imaging Assays for Chronic Kidney Disease.
You can view all of Kathryn’s articles here.
For more information contact us.
Interested in the scientist behind the in vitro glomerulus model?
Meet Dr Kathryn GarnerShare on social media:
Don't miss out on our latest innovations: follow us on Linkedin




